Gone are the days of “Just getting your bell rung”
This past week was absolutely crazy for me in terms of various webinars and zoom meetings as it was National Coaches Week in Canada. I took advantage of the various webinars, virtual conferences, summits during the day, and at night was participating in Zoom meetings to prep for online delivery of Hockey Canada NCCP clinics for BC Hockey due to COVID-19.
A couple of the sessions I did was attend a presentation on concussion management and the following day had a great chat with the director of an organization based in Florida who is providing Hyperbaric O2 Therapy to help people recover from brain trauma that I will expand on below.
Both of which really resonated with me personally as I probably suffered a few minor concussions during my playing days of tackle football when was hit helmet to helmet or tackled really hard. I recall a few times over the years when that would happen and I would be sitting or lying on the field woozy from the impact and trainers would run on the field to help me.
The first thing that they did was pull smelling salts out of their first aid kits and swipe under my nose where I would become more coherent and then they would say “Hey Bud, you’re good, you just got your bell rung” then help me back to the sidelines.
Then the head coach would come to me and ask me how I was doing and like players were doing for many years until recently where mandatory medical or return to play protocols were implemented and my response would be “I’m Good Coach” (but was I??)
To which they would say … Good to hear, Get back out there.
Fast forward many years later while running clinics, workshops or presentations across Canada interacting with coaches and other youth sports stakeholders may feel that the increasing concussion rates are attributed to the fact there is so much awareness now than it was in my playing days.
To which I say … I am glad that is the case because not only did I “probably” have a few minor concussions playing contact sports (none were diagnosed), I did have 2 Grade 3 concussions (most severe), the second ended my competitive playing career in contact sports in my 20’s.
Ironically it, like the first, were not from sports, rather were are result of bar brawls, the second I can only share what people told me after the fact as I lost approximately 2 weeks of memory leading up the incident and vague tidbits the days that followed.
In sum, I was doing a pub crawl with my buds for a stag and the one that was getting married was hit over the head with a beer mug and knocked out to which I came to his aid and I in turn was hit over the head and knocked the ground.
I literally had the S..T kicked out of me by three young men and I was taken to hospital, was in and out of consciousness per the doctors when I finally game to a couple of days later with what felt like a knife digging into my head …
The days, weeks and months that followed were extremely tough on me as doctors said I had to limit any activity, keep the lights off, rest while I recovered from the migraines, headaches, dizziness, nausea and other symptoms as a result of the concussion.
The incident happened in July and I was returning back to my second year of college and had to reach out to my advisor and instructors to advise that I could not return until I had the green light, that did not happen until early November.
I missed two month of my third term (of 4) in a really intense program but my instructors and fellow classmates were amazing helping me return and get back up to speed.
I share this as I know what it is like to deal with a major concussion, it is tough not only physically, but mentally as you are unable to do things I just took for granted, running, biking, hiking, playing sports, swimming, skiing, golf and so on.
So when coaches say to me the only reason so many more concussions are being diagnosed is due to awareness now vs in past I reply … I would rather doctor’s, coaches err on the side of caution.
I also have had players on teams I coached suffer concussions, one of the ones to this day I regret agreeing to let him return to play as soon as he did (even though he had doctor’s approval) was one that sustained a bad concussion in a game, came back a month later and sustained another concussion.
I received a call from his father later that night saying the doctor had advised that his son not play the remainder of the season and that he no longer play rep/competitive hockey with body checking as a result.
Although everyone said it was not my fault, I still feel some of the blame as I could have pushed back to his parents more and said give it more time but they insisted he was good to go.
This is why I was excited when I attended the webinar and talked with Hilary Loftus this week in terms of advances that the medical profession has made in terms of concussion management and recovery

Tina did a great presentation highlighting what concussions were, the ways that the can now be diagnosed by coaches and trainers utilizing concussion recognition tools like the one below
There have also been changes in terms how concussions are managed when diagnosed
- Complete rest for 48-72 hours is no longer advised in lieu early return to light activity that does not increase symptoms
- Slowly return to play/learn or work in terms of a graduated approach
Yikes … I potentially could have saved myself of 2+ months being in a dark room and literally doing nothing during that time?
She also shared following stats
- Most people recover quickly and fully
- 85-90% within 3 weeks
- Children take a little longer 4 weeks
Only 10-15% may have persistent symptoms (months to years), which mine as well as Sidney Crosby’s example as well as many other professional athletes who took months to return or had to retire as a result of concussions (i.e. Eric Lindros, Paul Kariya)

The Key takeaways that Tina ended her presentation for Coaches
- Know your athlete
- Be Supportive
- Community with the health care team managing the concussion if need quidance how to be supportive
- Speak the same language as the health care team
The day following Tina’s webinar, I had an opportunity to chat with Hilary Loftus, the director for HOW (Helping Our Wounded) Foundation which was established initially to help US military and veterans recover from brain trauma and PTSD using Hyperbaric Oxygen Therapy (HBOT)
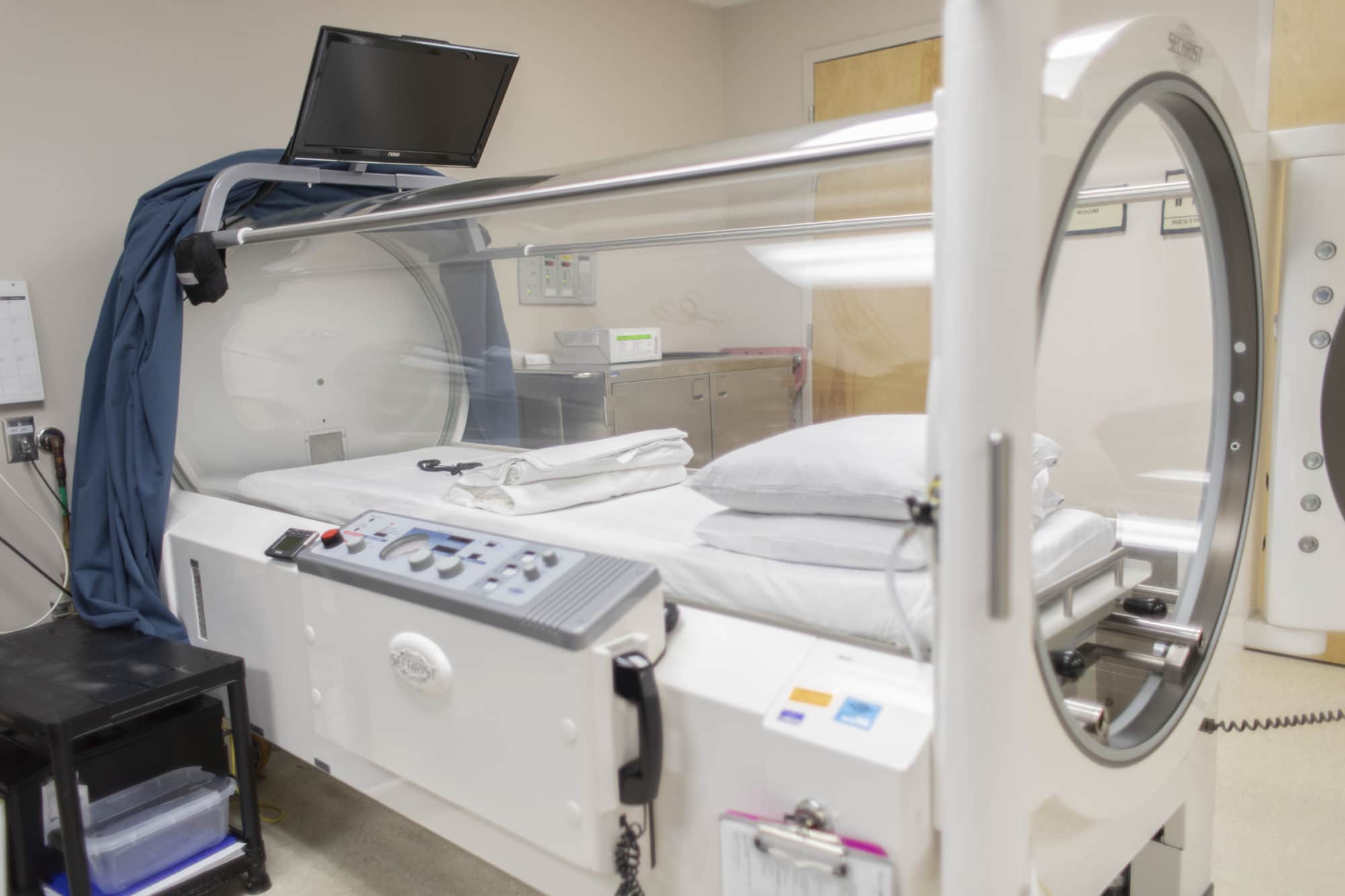
The sessions are either done in mono type chambers like the one above or they have larger ones that can accommodate groups of 4-8 or 12 at a time.
Pure O2 affects the body at a cellular level and by using pressured chambers it enhances and provides the tools for the body to naturally heal. A session is 80 minutes and the technology has been around for decades used mainly in hospitals for severe injuries, burns etc but is now becoming more mainstream in conjunction with other injury therapy practices (i.e. physical, occupational therapy)
Hilary shared an amazing stat with me also, if athletes who are diagnosed with a concussion start HBOT sessions within a week of being diagnosed they only have to do 3 sessions to recover and return to normal activity.
All I could say to myself during our chat and prior conversation was “I wish this was around for me many years ago” but it is exciting to see the advances that we are seeing for concussion management both in terms of recovery but ultimately in terms of prevention as many sports have implemented training programs for coaches, players to reduce head contact and severity of concussions many suffered in past.
If you are a coach and suspect one of your players has had “their bell rung”, that should be a red flag for you to immediately pull them from the field, ice, court and reach out to their parents to get them checked out and follow return to play protocols accordingly.
As the cliché goes, it is better to be safe than to be sorry.



